Asia Cervical Cancer Diagnostics Market Set for Strong Growth as Awareness, Screening, and Technology Reshape Women’s Healthcare
From Pap smears to HPV DNA testing, Asia’s cervical cancer diagnostics landscape is evolving rapidly—and that shift could save millions of lives.
Cervical cancer remains one of the most preventable yet persistent health threats facing women across Asia. For years, delayed diagnosis, limited access to screening, and low public awareness allowed the disease to progress silently in millions of cases. But that story is beginning to change.
Across the region, governments, healthcare institutions, diagnostic companies, and advocacy groups are working to make early detection more accessible and effective. As screening becomes more integrated into women’s healthcare systems, the demand for cervical cancer diagnostics is expanding steadily.
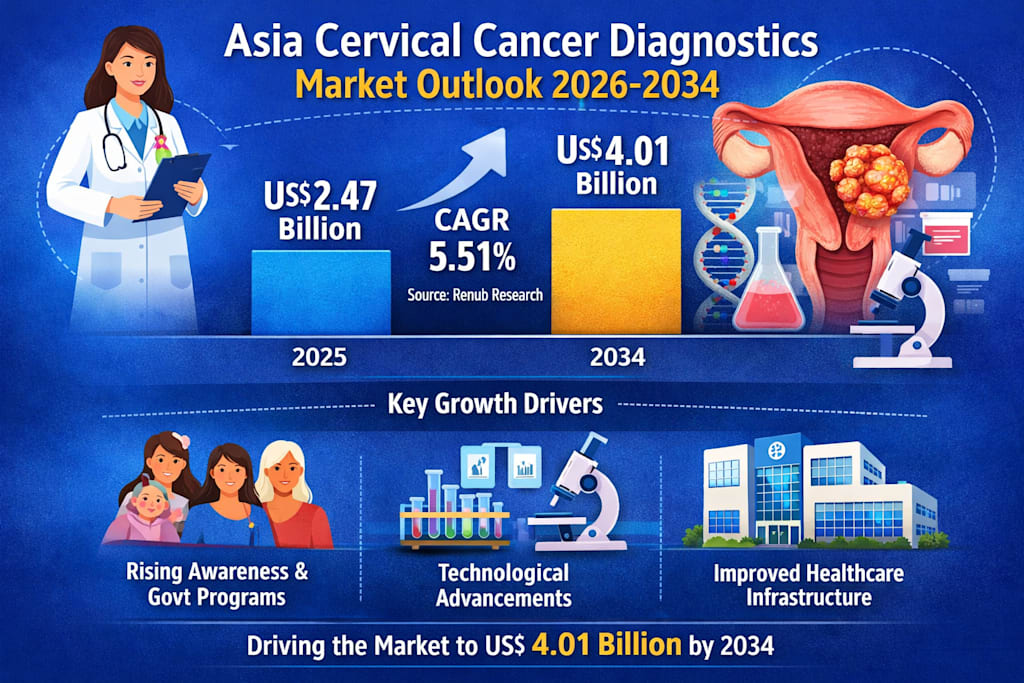
According to Renub Research, the Asia Cervical Cancer Diagnostics Market is projected to grow from US$ 2.47 billion in 2025 to US$ 4.01 billion by 2034, expanding at a CAGR of 5.51% from 2026 to 2034
That growth reflects more than just a business opportunity. It points to a larger shift in how healthcare systems across Asia are approaching cancer prevention, early diagnosis, and women’s long-term well-being.
Why Cervical Cancer Diagnostics Matter More Than Ever
Cervical cancer does not usually appear overnight. In most cases, it develops gradually through precancerous changes in the cervix, often caused by persistent infection with high-risk strains of the human papillomavirus (HPV). That means one thing is especially important: timely diagnosis.
Diagnostic methods such as Pap smear tests, HPV DNA tests, colposcopy, biopsies, and visual inspection with acetic acid (VIA) are crucial for identifying abnormal cell changes before they become life-threatening. The earlier these abnormalities are found, the greater the chances of successful treatment and survival.
This is exactly why the market is gaining momentum. Cervical cancer diagnostics are no longer being seen as niche clinical tools reserved for urban hospitals. They are increasingly being recognized as essential public health instruments.
In Asia—home to some of the world’s largest and most diverse populations—the need is particularly urgent. The region includes countries with advanced healthcare systems alongside areas where women still lack access to even the most basic gynecological screening. That gap is now driving innovation, investment, and policy reform.
Government-Led Screening Programs Are Driving Real Change
One of the biggest reasons behind market growth is the increasing number of government-supported cervical cancer screening programs across Asia.
Public health agencies are gradually moving from reactive cancer care to preventive screening strategies. In many countries, cervical cancer awareness campaigns are helping women understand that regular screening can detect problems long before symptoms appear.
This shift is important because awareness has historically been one of the weakest links in cervical cancer prevention. Many women in Asia—particularly in rural or underserved communities—have not traditionally undergone routine screening due to lack of information, social stigma, or limited healthcare access.
That pattern is slowly improving.
National campaigns are encouraging women to participate in Pap smear testing, HPV screening, and other low-cost diagnostic programs. These efforts are becoming more effective when combined with community health workers, public hospitals, local NGOs, and mobile health outreach services.
There is also growing international collaboration around cervical cancer elimination in the Indo-Pacific region, reinforcing the urgency of prevention and early detection. These initiatives are helping elevate cervical cancer diagnostics from a specialist medical concern to a mainstream healthcare priority
Technology Is Redefining How Screening Happens
The cervical cancer diagnostics market in Asia is not just expanding—it is becoming more advanced.
Traditional screening methods remain important, but the rise of high-sensitivity HPV DNA testing, molecular diagnostics, liquid-based cytology, and automated screening platforms is changing the quality and speed of diagnosis.
These innovations matter for several reasons.
First, they improve accuracy. HPV DNA tests, for example, are highly effective in identifying high-risk virus strains linked to cervical cancer. That allows clinicians to detect risk earlier, sometimes before cell abnormalities even become visible through conventional methods.
Second, modern diagnostic platforms improve efficiency. In high-population countries, automation and digital imaging can help reduce workload pressure on laboratories and minimize human error.
Third, and perhaps most importantly, new technologies are improving accessibility.
The development of point-of-care diagnostics and self-sampling solutions could be a game changer for women in remote or low-resource settings. These tools reduce dependence on centralized lab infrastructure and may help bring screening services to women who otherwise would not participate at all.
As technology becomes more affordable and scalable, the region is expected to witness wider adoption of modern diagnostic solutions—especially in urban and semi-urban healthcare systems
Healthcare Infrastructure Improvements Are Supporting Market Expansion
Another powerful force behind the market’s growth is the broader improvement in healthcare systems across Asia.
Many countries are investing in:
New hospitals and women’s health clinics
Expanded diagnostic laboratory networks
Better-trained healthcare professionals
Stronger primary care and cancer referral systems
These developments are making it easier for women to access regular cervical cancer screening as part of routine healthcare rather than only during emergencies.
Urbanization is also playing a role. As more women gain access to private healthcare, employer-sponsored medical checkups, and urban diagnostic centers, screening participation tends to rise. At the same time, outreach models such as mobile screening vans and community-based health programs are helping extend services into lower-income and rural populations.
This combination of infrastructure growth and public health outreach is creating a stronger ecosystem for cervical cancer diagnostics across the region.
Pap Smear Testing Still Holds a Powerful Position
Despite the rise of advanced molecular diagnostics, the Pap smear remains a cornerstone of cervical cancer screening in Asia.
That is not surprising. Pap smear testing has been used for decades, is relatively cost-effective, and remains widely accepted by clinicians and health systems. It is especially valuable in public health programs that need affordable screening solutions at scale.
In many Asian countries, Pap smear tests are already integrated into routine gynecological visits and women’s preventive health checkups. The market continues to benefit from:
Established clinical trust
Availability of trained cytology professionals
Lower cost compared to some advanced tests
Inclusion in public health screening initiatives
At the same time, the segment is evolving. In urban hospitals and advanced diagnostic centers, liquid-based cytology is increasingly being adopted to improve sample quality and laboratory efficiency.
So while newer technologies are gaining attention, Pap smear diagnostics are unlikely to disappear anytime soon. In fact, they will likely continue serving as a foundational screening tool for millions of women across Asia.
HPV DNA Testing Is Emerging as a High-Growth Segment
If Pap smears represent continuity, HPV DNA testing represents the future.
This segment is expanding quickly because it offers a more sensitive and increasingly preferred approach to cervical cancer screening. Rather than detecting only visible cell abnormalities, HPV DNA testing identifies the presence of high-risk viral strains responsible for the majority of cervical cancer cases.
That matters because it allows earlier intervention and better risk management.
The benefits of HPV DNA testing include:
Higher sensitivity
Earlier detection of risk
Longer screening intervals
Better integration with preventive screening programs
As awareness of the link between HPV and cervical cancer grows, this diagnostic segment is becoming more accepted in both public and private healthcare settings.
Cost has historically been a barrier, especially in lower-income regions. But as test prices decline and awareness increases, adoption is expected to accelerate significantly in the coming years.
This is particularly relevant in countries such as India and Malaysia, where the market is beginning to reflect a stronger demand for modern, reliable, and preventive diagnostic options
VIA Remains Essential in Rural and Resource-Limited Areas
While advanced testing gets much of the attention, VIA (Visual Inspection with Acetic Acid) continues to play a highly practical and important role across Asia.
VIA is simple, inexpensive, and can often deliver immediate results. That makes it especially valuable in settings where laboratory access is limited or where healthcare systems need to screen large populations quickly and affordably.
In countries with vast rural populations, VIA remains a highly effective public health tool because it:
Requires minimal equipment
Can be performed in community settings
Supports rapid screening and referral
Helps expand access where lab-based testing is limited
Although it is less specific than molecular tests, VIA remains indispensable in low-resource environments. For many women, it may still be the first and only screening option available.
That makes it not just relevant, but essential.
Country-Level Growth Stories Are Shaping the Regional Market
The Asia cervical cancer diagnostics market is not moving as one uniform block. Different countries are contributing in different ways.
China
China’s market is benefiting from large-scale public health programs, a growing emphasis on women’s preventive care, and improved urban diagnostic infrastructure. Pap smear testing remains widely used, while liquid-based cytology is gaining traction in higher-capacity facilities.
Japan
Japan represents a more mature and clinically advanced market, with well-established screening systems and high standards in laboratory diagnostics. Pap smear testing continues to hold a strong place in routine health checks and workplace wellness programs.
India
India stands out as one of the most dynamic growth markets. Rising awareness, expanding private healthcare, and increasing interest in HPV DNA testing are helping reshape the screening landscape. At the same time, VIA remains critical for reaching underserved populations.
Malaysia
Malaysia is experiencing steady adoption of HPV DNA testing, supported by improved healthcare access, expanding molecular diagnostic capabilities, and a stronger focus on early detection.
Thailand
Thailand’s VIA segment remains especially important in improving screening coverage in rural and lower-resource areas, reinforcing the country’s public health efforts to reduce cervical cancer mortality
Challenges Still Need to Be Addressed
Despite the market’s positive outlook, serious barriers remain.
One of the biggest challenges is limited awareness, especially in conservative or underserved communities where social stigma and misinformation can prevent women from seeking screening.
There are also major disparities in healthcare access. Urban women may have access to modern diagnostic centers and advanced testing, while rural populations often face shortages of trained staff, laboratories, and affordable screening options.
Cost is another important issue. While technology is improving, affordability still determines whether diagnostics can truly reach mass populations.
In short, growth alone is not enough. The region must also ensure that progress is inclusive, equitable, and practical.
Final Thoughts
The Asia Cervical Cancer Diagnostics Market is growing because the need is real, urgent, and long overdue.
This is not simply a story about market expansion. It is a story about women gaining better access to life-saving preventive care. It is about healthcare systems moving earlier, smarter, and more efficiently. And it is about a region increasingly recognizing that early diagnosis is one of the strongest weapons against cancer.






Comments
There are no comments for this story
Be the first to respond and start the conversation.